SPECIAL HOSPITAL SVETI VID has introduced new era of glaucoma surgery, changing old and non-efficient surgical procedures.
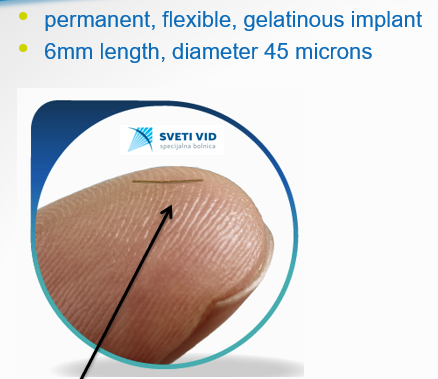
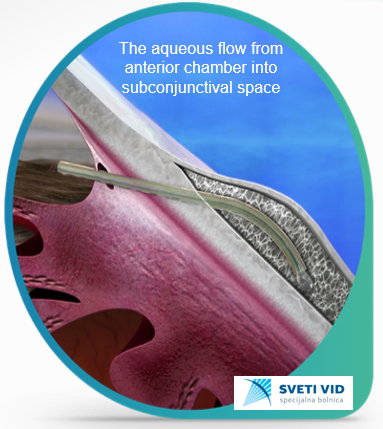
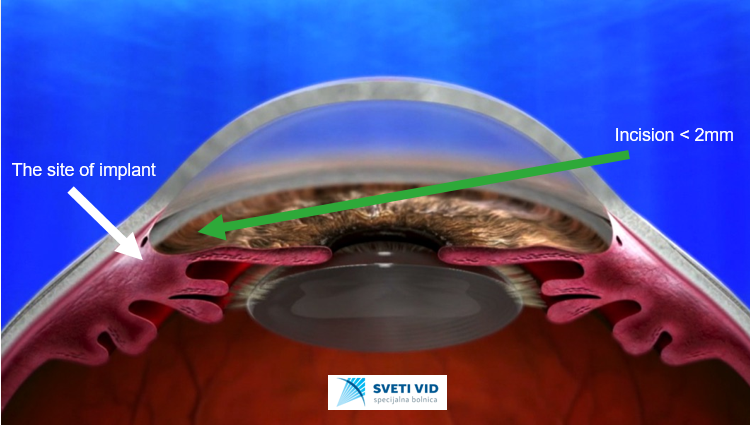
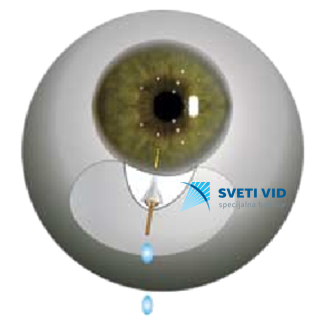
This new era has started with new method using miniature intraocular implants (MIGS), after which the patient achieves new comfort in life, without using eye drops, which makes a big difference comparing to old methods when patients suffered from allergic reactions on eye drops.
In special hospital SVETI VID this surgery is performed by experienced European surgeons, who have special license which is necessary for performing this type of surgery.
Glaucoma in the widest sense implies a group of diseases resulting in damage of the optic nerve with loss of visual function and ultimate blindness, if not treated. These diseases are MULTIFACTORIAL with a wide range of risk factors where the elevated intraocular pressure is only one of them.
Symptoms
Most frequently it is chronic and begins insidiously, without noticeable symptoms in the beginning, painless, yet leaving alarming number of blind people of various age.
When confronted with diagnosis, patient first reaction is unbelief. The sight initially has not been compromised. Elevated intraocular pressure, as most frequent manifesting sign of disease, except in twice increased then normal values, does not bear pain.
In acute condition, accompanied with high intraocular pressure, the eye is “hard on touch”, painful, with severe pain spreading toward the entire half of the head, followed by nausea and vomiting.
Glaucoma strikes first at peripheral vision, therefore the peripheral visual field defects are detected, whereas central vision remains preserved. That is why the first symptoms are “silent”. When the pain occurs and visual field defect becomes apparent, the significant irreversible damage to the optic nerve has already occurred.
At this moment the target of the therapy is to halt the disease at present stage, and keep the intraocular pressure under control. It is essential to demystify the problem and help the patient understand the disease, because only then he will understand the necessity for timely treatment. Glaucoma is lifelong, but prompt and proper care will make possible normal life with a disease that is kept under control (such as high blood pressure).
When glaucoma develops
The contemporary ophthalmology means detection, as early as possible, of the initial symptoms and signs of possible glaucoma, and thereafter with wide range of subtle diagnostic procedures, to confirm or exclude the disease, at the moment.
At the earliest stage there are changes on the level of the retinal ganglion cells!
There are many predisposition factors and risk factors for development of some of a few types of glaucoma.
Basically, there is a defect in vascular supply because of perfusion disorders, upon which the neural cell is highly sensitive. Its sensitivity is greater in cases of elevated IOP or oscillations in the IOP. Perfusion disorders exist with circulation problems, such as carotid arteries stenosis, decreased blood pressure and high myopia respectively.
These risk factors can intensify the damage, yet all this means not that all patients with circulation problems necessarily have glaucoma. Genetics will dictate the behavior and sensitivity of these fine structures in the frame of all present risk factors.
Risk factors
Increased IOP is considered the main risk factor, but not the only one.
Old concept that increased values of intraocular pressure with optic nerve damage and typical glaucomatous “defect” in visual field constitute glaucoma is somewhat deficient and has changed today. Increased IOP will accelerate the development of glaucomatous damage, yet glaucoma IS NOT the same as increased intraocular pressure, by itself. Some records show fine changes in the optic nerve structure at the back of the eye (papilla) in conditions of “relative” normal or even lower IOP.
That is so called normal or low- tension glaucoma. Values of IOP from 9-21mm Hg are taken for ‘’normal’’ by concensus, which means that 95% of people without glaucoma have the values with that range of IOP. The rest without glaucoma can have higher or lower values than above mentioned. Anyway, comprehensive diagnostics are necessarily to exclude glaucoma.
Around 25% of patients with clear glaucomatous defects has pressure within “normal”. That means that the absolute values of IOP cannot be interpreted without necessary data, which means: the grade of damage, positive hereditary anamnesis, the presence of other risk factors, oscillation of IOP during the day etc.
The asymmetry of ocular pressure between eyes, and higher daily fluctuations of pressure are alarming sign, as well as existing asymmetry in PNO appearance even within “normal” values of IOP.
Heredity
Verified damage of the optic disk, or visual field defect, as well as positive family history for glaucoma is an alarm to re-examine whether the measured IOP is the optimal for that person, itself, or has to be lowered.
Therapeutic action is taken when even subtle changes are detected.
Glaucoma types
Elevated eye pressure (“hard eye”) occurs because of disbalance in production and drainage of aqueous humor. Greater production in relation to drainage, respectively harder drainage because of increased resistance in “canals” through which aqueous flows, at normal eye anatomy and angle chamber structure is characteristic of so called open angle glaucoma.
Difficult drainage occurs in conditions of altered chamber angle (narrow or closed angle glaucoma) which can be congenital, or the anatomy is changing with age. Farsightedness with shallow eye chamber is predisposition for glaucoma as well. Secondary glaucoma occurs in ocular inflammations (uveitis) or traumas, because of inflammatory debris in angle chamber. It can be expected as a complication of „maturing“ of cataract, when swollen lens narrows the anterior chamber and angle, or obstructs pupilary region and cuts off the flow of aqueous humor from posterior into anterior chamber.
Should it disintegrate, this cataract can lead to clogging of the chamber angle or secondary inflammatory reaction – uveitis. These all are dangers of obsolete concept about „waiting to mature“ abandoned in ophthalmology in the seventies of the past century. Prevention measurement is an early cataract surgery- phacoemulsification (ultrasound surgery).
UNFAMILIAR WORDS:
IOP –intraocular, eye pressure
Papilla of the optic nerve, PNO, optic disc – the beginning, the head of the optic nerve
Perfusion – blood supply to the tissue