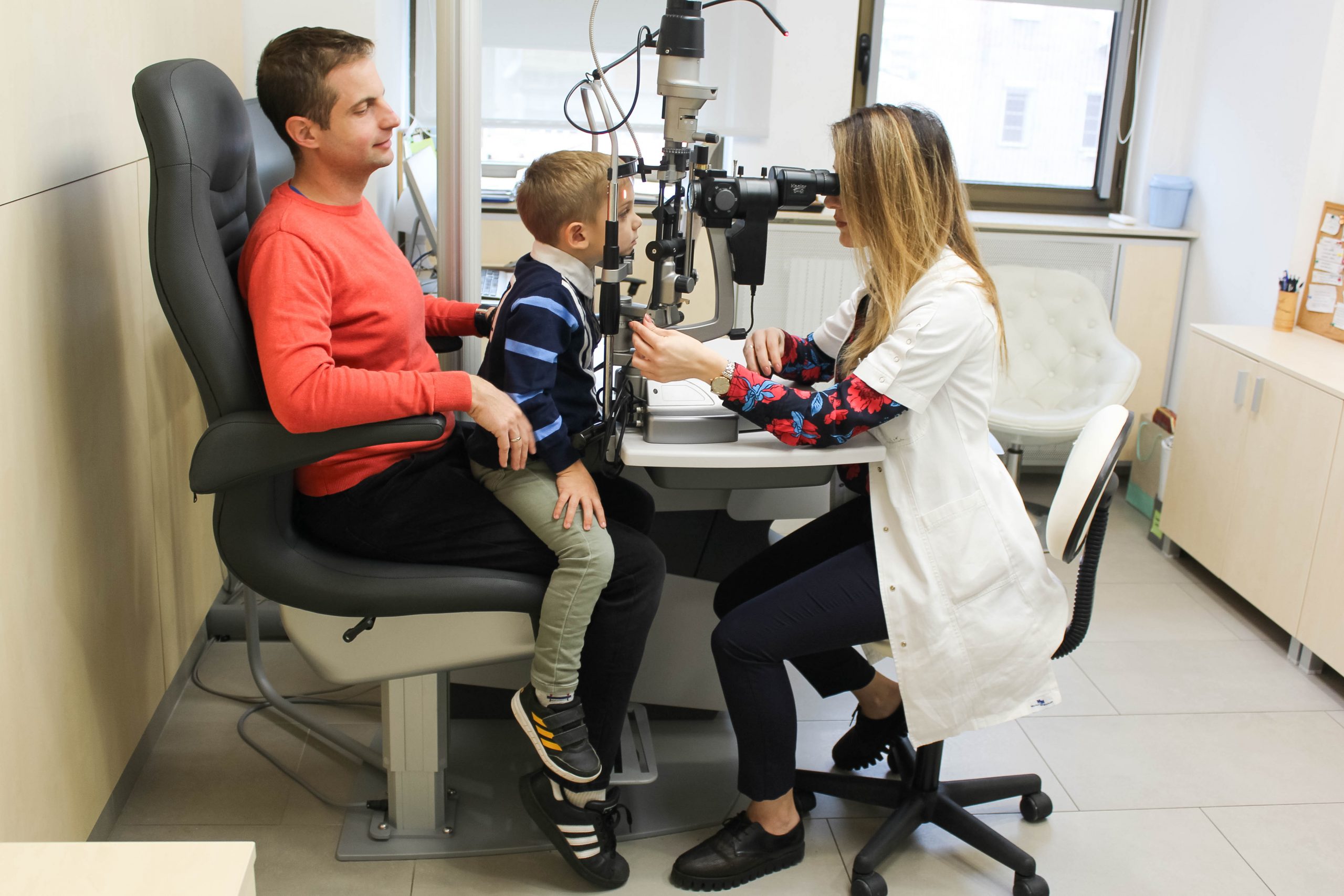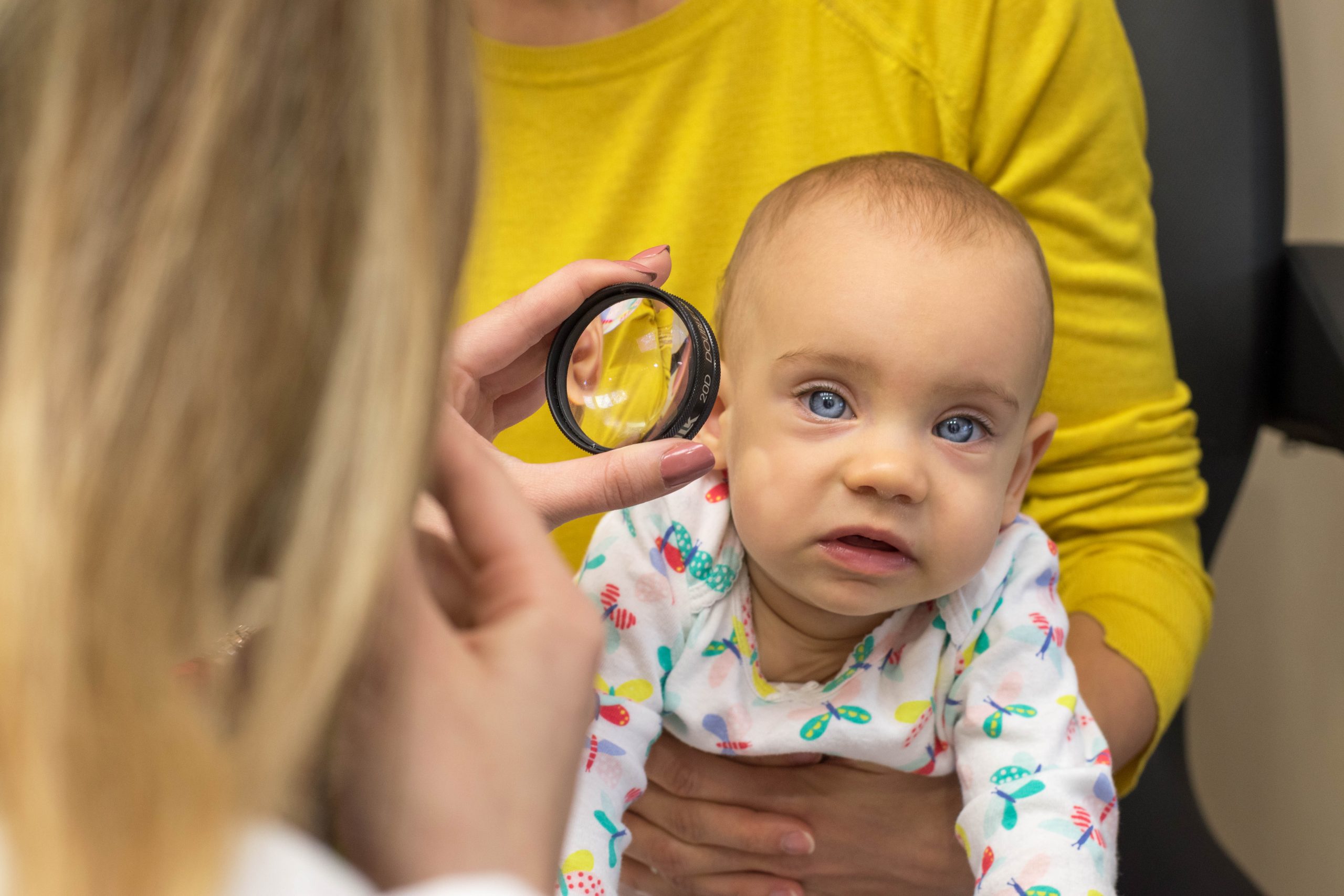
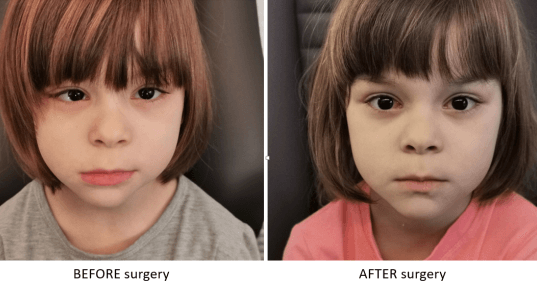
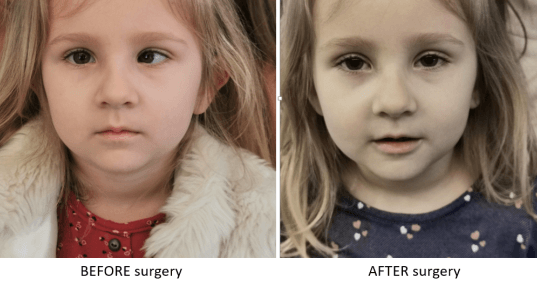
Congenital cataract is a burden for visual development and causes amblyopia. If the lens is completely opacified, light cannot enter the eye and there will be no vision.
Amblyopia develops very quickly, especially if cataract is only in one eye, and when the urgery is delayed.
Early cataract surgery in babies, aged a few months, gives the condition for visual development.
Adequate intraocular lens (IOL) which will correct the refractive error, will be implanted in the same eye, and will stay in the eye for the whole life.
The adequate IOL will be chosen concerning the age of a child at the time of operation, findings on examination and potential for high pseudophakic myopia development, which means that after cataract surgery it is possible to find myopia development, as the eye starts to be in use.
With IOL implanted (pseudophakia), better correction and visual development is achieved, than in the case of surgery without IOL implantation (aphakia) with postoperative correction of high dioptry with glasses (‘’thick’’ glasses).
In rare situations, the eye will stay without lens implant: small non-developed eye (nanophthalmus), anterior segment dysgenesis, inflammation.
After the operation, regular follow-ups are suggested, after a week, month, 3 and 6 months, then yearly, in order to perform the pleoptic treatment against amblyopia.
As the child is growing, after a few years will be necessary to recorrect the refractive error with glasses, contacts or laser. That is the age of already achieved improving in visual acuity and additional correction will even make it better. Of course, that is not as high refractive error as it might have been, if previously IOL had not been implanted during the cataract surgery.
If cataract is not dense and visual axes is clean, the light is able to pass through the lens, as it is a stimulus for visual development. That means that the danger for high amblyopia is less, and it is possible to wait for the operation till the moment when vision worsened.
The human lens in young has the role in accommodation, and that is why there is no need to hurry with operation.
In the case of traumatic cataract, the surgery should be done as soon as possible.
When planning the operation in cases with low level of amblyopia, multifocal implant should be an option. This implant might be the substitution for lost accommodation, giving acceptable near, intermediate and far vision.
Congenital cataract surgery in early age will give the chance for visual development, but intensive amblyopia treatment after the operation is a must!
Closing the better eye, or alternatively both eyes, will train the weaker eye to take the function and to develop binocular vision.
CONGENITAL GLAUCOMA is a serious eye disease for the whole life that will end in blindness, without appropriate operation and complete treatment, that will last for the whole life. It could be discovered immediately, on birth, or later. It is not rare that parents themselves, discover the ‘’big eye’’, eye ball is protruded and the cornea is very large and thin, but very soon opacity on cornea could be seen, what makes parents urgently asking for help.
The eye ball layers are very elastic in children, and in the case of high intraocular pressure (IOP) the enlargement of eye ball can compensate high IOP in some way, and it will somehow, for a while, protect the optic nerve.
The only treatment is surgery and drops, afterwards.
Congenital glaucoma very often goes with congenital cataract and some other anomalies of anterior segment of the eye (iridocorneal touch, iridocorneal dysgenesis, coloboma iridis, aniridia,…).
This is the disease for the whole life, despite the surgical procedure, requires constant follow-ups and possible medical or laser treatment, or another operation.
In congenital anomaly as dysgenesis of anterior segment, nanophthalmus (small eye), glaucoma is following risk, that makes the prognosis bad and requires frequent control for the whole life.
For patients with small eye (nanophthalmus) in late ages, when glaucoma risk becomes manifest (because of a shallow anterior chamber), surgery on the lens – phacoemulsification is the way to regulate the high intraocular pressure by making anterior chamber deeper.
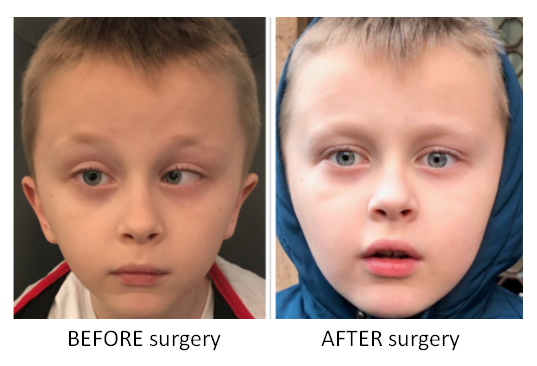
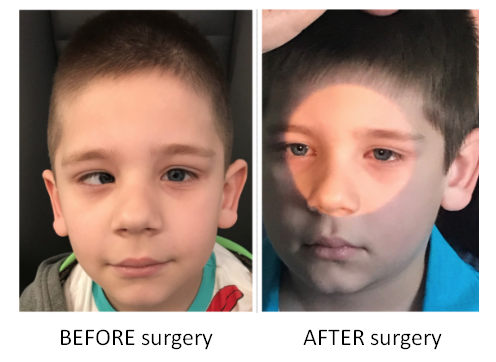
STRABISMUS (CROSSED EYES) is very easy to recognize in children. It is the deviation in positioning of eye balls. The normal position of the eye balls is as important factor for binocular visual development and stereopsis, as good refractive error correction.
If it is diagnosed immediately on the birth, or a few months after, then early treatment is of crucial value for better postoperative prognosis in development of visual acuity and binocular vision. Of course, before the strabismus operation, it is necessary to exclude the possible other causes of crossed eyes (neurological reasons, tumor, cataracts, etc.).
After the operation, if there is a refractive error present, it should be corrected with glasses or with excimer laser, and pleoptic treatment is a must.
Strabismus could be classified in various subgroups, depending on the axes of eye ball position (horizontal, vertical, oblique misalignment). As congenital, it is often presented in paralythic, restrictive or special syndroms (Duan, Mebius, etc.).
Accommodative strabismus is a kind of eye misalignment that could be corrected with full refractive error correction, not with strabismus surgery. That is because of very strong accommodation, which makes the eyes crossed. The aim of refractive correction is to ‘’relax accommodation’’. That could be achieved with glasses or laser surgery, which is the better way for complete removal of refractive error.
UNDERSTANDING THE NEEDS
Refractive surgery in children is in practice for many years. It is the right choice in specific situations, when development of amblyopia is threatening at the age critical for visual acuity development, and refractive anomaly cannot be corrected by conventional means. Those amblyogenic situations, leading to “functional blindness” are following:
When there is high degree of myopia, hyperopia or astigmatism on both or one eye (big difference in diopter value between eyes), without possibility of achieving good correction with standard approach, because of lack of cooperation with small child or contact lens intolerance, or absence of positive answer to wearing glasses (limiting possibilities of glasses in these cases) and that in the period of most intensive development of visual function.
Children with special needs and high myopia accompanied with other ocular (albinism, prematurely born children etc…) or medical problems (autism, Down Sy, cerebral paralysis and other neuromuscular diseases etc…), where standard approach is inefficient or impossible to achieve. In these situations, without laser correction these children remain “functionally blind” or with very limited visual function, and that is one more stigma burdening already difficult psychosocial status of these families.
Accommodative strabismus, with big amblyogenic potential, to provide persistent adequate correction.
The goal of refractive procedures in children is not getting rid of glasses dependence or contact lenses as with adults, where the visual function development has already taken place. This is a chance to reduce anisometropia in children and manage balance between both eyes and gain isometropia (balanced diopter values), to completely correct high refractive error, much better than standard treatment and that way enable better development of visual function, better quality of visual acuity and binocular- stereo vision. In this way even better cooperation is obtained with child accepting mandatory treatment for amblyopia by covering the better eye.
At the age critical for development of visual function (until the age of eight), full correction of refractive error is imperative. Some children manage correction with spectacles, some with contact lenses (rarely, because of age or intolerance), and some of them remain with inadequate correction, what often results in amblyopia and strabismus.
Big difference in diopter value in both eyes is potentially amblyogenic anomaly, leading to amblyopia respectively. That means that in situations when constant and adequate correction is not achieved, the eye with high diopter will stay “neglected” in comparison with “better” eye by which is fixating and which will become dominant eye. Difficulties in correcting high prescriptions in glasses or contact lens intolerance, and poor cooperation respectively, the only therapeutic approach that will enable better, sharper image and correct the quality of life of these children is refractive surgery. Here, the goals are far than simple solutions of dioptric problems in older, with already developed visual function and cultivated sight, where by laser “removing of the diopter” ends the dependence from glasses and contacts.
Refractive surgery in pediatric age (especially below the age of 8years), offers excellent possibility of establishing isometric condition (balancing of diopter value) on both eyes, if anisometropia or bilateral highly amblyogenic error (one leading to amblyopia) in situations of high myopia, hyperopia or astigmatism. That way it is achieved better quality, more natural and sharper image and possibility of establishing binocular-stereo vision, because the brain will receive same or similar images easy combined into one, rather than when having two different quality images as in glasses correction, which in these cases are not optimal solution. Intolerance is partially connected to physiological moments of not adapting to glasses, because of difference in size and shape of images received from both eyes as well as space and depth perception, therefore the development of binocular vision is hindered.
Often in practice it is opted for intentional under-correction of diopters aiming to get close to the “better” eye, but by that conditions for development of amblyopia are not removed. It is impossible to manage cooperation with small child to accept contact lens, as the contact lens itself can cause numerous problems for cornea. These problems are overcome with refractive surgery. Results of many years have shown the efficacy of pediatric refractive procedures, applied at earlier age, in mentioned indications when amblyopia is unavoidable.
Refractive surgery presently is performed as therapeutic procedure. In mentioned situations which present clear indication for laser procedure, today the time is not wasted with glasses, but immediately the children are recommended laser correction already at two years of age, with controlled treatment of covering the better eye for certain number of hours daily or alternate covering after laser procedure. It is implied that modern laser technology with necessary preoperative preparation in adequate surgical environment, in general anaesthesia with trained team and surgeon with great experience in these procedures. The other way to achieve target in these indications, when laser is not indicated because of thin cornea or extremely high diopter, is the surgery of implanting phakic intraocular lenses, by which the natural, biological lens and act of accommodation is preserved.
This procedure is indicated in very high diopters above +6 D of hyperopia and myopia above-13 D, and with corneas too thin for laser procedure, and with adequate anterior chamber depth as essential premise. It is performed in general anaesthesia.
Refractive pediatric surgery is performed in the world in certain medical indications, as listed above, form many years, in several world leading university pediatric clinics, with high level of surgery and long period of practice. From these institutions, as from works of Professor Autrata, came out these procedures as regular, highly positively accepted, with stable, predictable and safe results (clinics in Houston, Washington, New York, Calgary-Canada, Alicante-Spain, Great Britain, Italy, Czech Republic…).
Among them is Special Hospital Sveti Vid in Belgrade, Serbia, with high level of pediatric ophthalmology and pediatric refractive surgery, with Professor Autrata as a member of the team, who set up here in Sveti Vid another great center of pediatric ocular surgery.
Refractive pediatric surgery in SVETI VID reffers to strict medical indications: high anisometropy or high bilateral myopia, hyperopia and astigmatism, with high amblyogenic potential, when conventional treatment with glasses or contact lenses failed.
We use, for safety reasons, superficial laser ablation methods (T-PRK SmartSurfACE )
Refractive range is approximately from -13 up to +6 D, regarding the age, corneal characteristics and complete estimation. We do not recommend LASIK because of risk and potential complications, even not for adults. Laser procedures are performed on Schwind Amaris Excimer Laser. For children is recommended to do this procedure in general anesthesia (inhalation) and analgo-sedation. In compliant children, topical anesthesia is used. Surgical environment is well-equipped, with highly-educated and experienced staff.
Refractive procedures in children are done by Prof. Dr Rudolf Autrata.
He is one of the leaders in the world of ophthalmology, and one of the most cited person devoted to refractive procedures in children from early 90-ties of XX century. He published numerous articles in high-indexed journals and was honored for great contribution to development of pediatric ophthalmology. He is a chief of pediatric eye hospital in Brno, Masaryk University. He was many times awarded on international congresses for his work. In Special Hospital SVETI VID, he works as a chief of pediatric department.
Surgical procedure, in application in cases of progressive nearsightedness in order to strengthen the eye covering, which is a risk of retinal detachment. This can not halt completely, but it can slow down further growth of nearsightedness and strenghten the structure, of already thinning eye covering. This decreases the risk of occurrence of retinal detachment.
It is performed in general anaesthesia, now with special biocompatible implants, in wide application in other medical fields as well (cardiac surgery, abdominal surgery etc.). There is no need to stay in the hospital, only several hours after surgery, then a child is released to go home the very same day after surgery.
First follow up is 3-4 weeks after surgery. After that there is period of monitoring and controls.
Development of high myopia (nearsightedness) mainly occurs because of progressive growth of the eye ball, along the axial length. Normally, in young people, the shape and curve of the eye lens will compensate this growth. That process is called emmetropization. Sometimes, that is not enough and growth of the eye ball surpasses the range of emmetropization, resulting in certain degree of nearsightedness. The tissue of the bulbar wall (eye covering) is thinning, and the appearance of the posterior segment, retina, begets specific “myopic” appearance, thinned and apt for defects, with all the risks from retinal detachment.
As surgical procedure, by which that progressive growth of axial length is halted, as well as progression of myopia, preserve the covering tissue from further thinning, strengthen its structure thereby decreasing the risk of retinal detachment, recommendation is SCLEROPLASTY.The procedure is in application for many years. It is performed in general anaesthesia, now with special biocompatible implants, in wide application in other medical fields as well (cardiac surgery, abdominal surgery etc.). There is no need to stay in the hospital, only several hours after surgery, then a child is released to go home the very same day after surgery.
First follow up is 3-4 weeks after surgery. After that there is period of monitoring and controls.
Reasons for developing high myopia are different: genetics, after pediatric cataract surgery, loss of normal compensatory mechanism of emmetropization of the bulbus, which is known and taken in account when determining the strenght of intraocular lens which will be implanted during the cataract surgery, considering the age (several months, up to six months, up to a year and older…) High myopia is also expected in some syndromes, such is Down syndrome, or in prematurely born children, where occurred regression retinopathy stage (ROP regression).
PTOSYS (DROOPING EYELID) in pediatric age if it closes central visual axis, therefore creating conditions for developing amblyopia, if exists prior to the age of four.Esthetic moment in pediatric age is not definitive and early surgery has meaning from the aspect of removing obstacles for visual function development..
CONGENITAL AND ACQUIRED CHANGES IN CORNEA
Today a great number of surface changes on cornea-opacities, scars, recurrent erosions with difficult healing, in children, as well as in adults are successfully solved with laser treatment – PTK (phototherapeutic keratectomy).
This therapeutic application of excimer laser removes the superficial-defective layer and facilitating its recovery, leaving fine, smooth surface of cornea. With this method subjective disturbances are diminished (pain, irritation, increased lacrimation, photophobia), and in combination with PRK method (photorefractive keratectomy) can simultaneously solve refractive problem of this cornea.
CLOGGED NASOLACRIMAL CANAL (tear duct). It is detected because of increased lacrimation of the eye and frequent infection (discharge). It is solved surgically by implantation of special drainage implant, allowing reestablishing normal fluid communication.
This implant is comfortable for children and after achieved “healing”, actually established communication it can be removed.
Amblyopia, the term derived from Greek language. It stands for poor vision, without possibility of sharpening it with glasses or contacts, yet without visible morphological changes. It is functional poor-vision. The causes for this exist from early childhood and if not detected timely and treated, they remain for good.
Amblyopia must be treated from early childhood, and for proper treatment it must be detected in time. It is of great importance for visual potential, because there will be no possibility of improvement after the age of 6, at the latest 8 years of age, depending on cause beneath it. Therefore, modern ophthalmology insists on strict controls of visual function in children and early solving of amblyopia.
MOST FREQUENT REASONS FOR DEVELOPING AMBLYOPIA ARE:
Strabismus (it can be result of amblyopia and/or its cause).
Anisometropia (difference in diopter value in both eyes) from early childhood that is not treated.
Refractive error (uncorrected diopter) in early childhood.
Congenital cataract, unoperated in early childhood
Treatment by occlusion